Graves’ disease, also known under the name Graves , is an autoimmune disease affecting the thyroid gland, which causes hyperthyroidism or hyperfunction of this gland. Graves’ disease represents 76% of hyperthyroidism in particular. It preferentially affects relatively young women, but it can nevertheless occur at any age.
A little history
Robert James Graves was an Irish surgeon. Having described exophthalmic goiter in 1835, he gave its name to Graves’ disease . Born in Germany on March 27, 1796, he died in Dublin on March 20, 1853.
Little reminder on the thyroid gland
The thyroid is a hormonal gland located next to the esophagus in the shape of a bow tie. It is also made up of a group of vesicles formed from a single cell layer, mainly composed of thyroglobulin. This thyroid essentially produces two main hormones: T3 (triiodothyronine) and T4 (tetraiodothyronine) or thyroxine, which play a key role in cell metabolism and energy production.(in the form of ATP). Another thyroid hormone: thyroid calcitonin, which is particularly linked to growth. It has also been shown that hyperthyroidism has a greater impact on young women than on men, and that it usually manifests itself in a hereditary (or genetic) form. However, it can also be the consequence of other diseases (such as diabetes mellitus).
Focus on hyperthyroidism
Hyperthyroidism can indeed cause an abnormally high secretion of thyroid hormones . The body of a person with Graves’ disease thus produces autoantibodies of the immunoglobulin type IgG . These antibodies targeting the organism itself are in particular permanently attached to the thyroid receptors for thyroid stimulating hormone or thyroid stimulating hormone TSH. Most patients therefore have these antibodies, called TSI: Thyroid Stimulating Immunoglobulins.
What is Graves’ disease?
Graves’ disease affects approximately 0.5% of the population and is responsible for most cases of hyperthyroidism (50 to 80%). As with hyperthyroidism alone, women represent the vast majority of those affected by this disease. Graves’ disease is therefore more common in young to middle-aged women, and the peak is between 40 and 60 years old, but it can still occur at any age.
This disease is autoimmune thyroiditis with genetic as well as environmental factors, both of which ultimately can easily lead to the onset of this disease. Certain subclasses of HLA class II genes have been identified as predisposing genetic factors, and a consistency of Graves’ disease was found in 35% of identical twins. A family history of Graves’ disease is actually associated with an increased risk of the disease and an older age of onset .
Usually, the proportion of T3 secreted by the thyroid is about 20% of the total, but in Graves’ disease it increases to about a third .
What should be done in the event of hyperthyroidism?
It is important to be screened for mild to early hyperthyroidism (TSH between 0.1 and 0.240 mIU / L), and overactive thyroid (TSH between 0.240 and 0.500 IU / L), which also require monitoring clinical and biological. An appropriate etiological assessment should be carried out to diagnose possible Graves’ disease or a hot thyroid nodule. At a minimum, a thyroid ultrasound is required, possibly a thyroid gland scan. Specialist advice may be necessary.
Before going to synthetic antithyroid drugs (carbimazole, thiomazole), it is always possible to start with a gentler curb in herbal medicine. In addition, the two therapeutic approaches can be complementary , always ensuring medical, clinical and biological monitoring.
What are the symptoms of Graves’ disease?
Hyperthyroidism is directly related to Graves’ disease and however can cause certain signs and symptoms, such as thermophobia, digestive disturbances, severe weight loss, feeling of tension and shaking, increased heart rate with tachycardia, respiratory failure, chronic fatigue, etc.
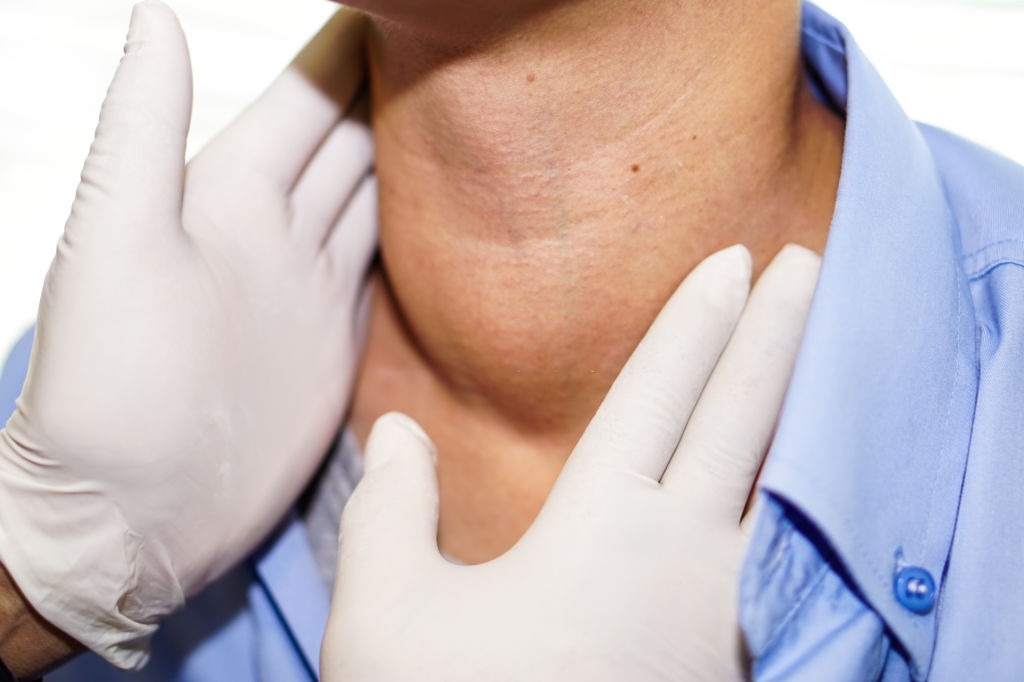
In some forms of Graves’ disease, these symptoms are sometimes associated with a large goiter , swelling of the skin on the legs, and eye disorders where the globes appear unusually large or “protruding” with a sensation of dry and burning eyes.
Where are we in terms of clinical research on natural treatments?
Blood dogwood :
In association with Viburnum lantana , Cornus sanguinea is an excellent hyperthyroid treatment (Graves’ disease) with signs of thyrotoxicosis, tachycardia, weight loss, tremors of the extremities, thermophobia, irritability, hyperemotivity, or even diarrhea.
The Grémil:
Grémil is endowed with antithyroid activity. It slows down thyroid function by different mechanisms :
- Inhibition of enzymatic deiodination of thyroxine T4 to triiodothyronine T3
- Inhibition of the uptake of iodine into the thyroid
- By combining with TSH, it thus opposes its action, without modification of the growth hormone
- Inhibition of intrathyroid adenyl cyclase activation
Lemon balm :
Indicated in mild hyperthyroidism, or even Graves ‘disease, extracts of Lycopus virginicus , Lycopus europaeus , Melissa officinalis , or even Lithospermum officinale , indeed have antithyroid activity and can interact with G immunoglobulins specific for Graves’ disease by inhibition of their binding to the TSH receptor capacity.
Nigella :
Nigella is further recommended in autoimmune diseases, such as multiple sclerosis, Graves’ disease, rheumatoid arthritis, systemic lupus erythematosus, Reiter’s syndrome, etc.
Medical bibliographic sources and clinical trials :
- Eiling R, Wieland V, Niestroj M. Improvement of symptoms in mild hyperthyroidism with an extract of Lycopus europaeus (Thyreogutt® mono). Wien Med Wochenschr. 2013
- Beer AM, Wiebelitz KR, Schmidt-Gayk H. Lycopus europaeus (Gypsywort): effects on the thyroidal parameters and symptoms associated with thyroid function. Phytomedicine. 2008
- Michael Auf’mkolk, Jonathan Car. Ingbar, Ken Kubota, Syed M. Amir, Sidney H. Ingbar. Extraits and Auto-Oxidized Constituents of Certain Plants Inhibit the Receptor-Binding and the Biological Activity of Graves ‘Immunoglobulins. Endocrinology, 1985
- Gheita TA, Kenawy SA. Effectiveness of Nigella sativa oil in the management of rheumatoid arthritis patients: a placebo controlled study. Phytother Res. 2012
- Sourgens H. et al., Antihormonal Effects. TSH and Prolactin-Suppressing Properties of Lithospermum officinale and other Plants, Planta Med, 1982
- Auf’mkolk M. et al., Inhibition by Car certain Plant Extracts of the Binding and Adenylate Cyclase Stimulatory Effect of Bovine Tryrotropin in Human THyroid Membranes, Endocrinology
- Winterhoff H. et al., Antihormonaleffects of plant extracts. Pharmacodynamic effects of lithospermum officinale on the thyroid gland of rats; comparison with the effects of iodide, Horn Metab Res., 1983
- Yarnell E. et al., Botanical Medicina for Thyroid Regulation, Alternative and Complementary Therapies, 2006
- Dhom G., Wernze H. On the antithyrotropic and antigonadotropic mechanism car of action of Lithospermum officinale. (Morphological studies of the rat hypophysis), Acta Endocrinol, 1963



A quick look at Grave’s disease
Graves’ disease is an autoimmune condition that affects the thyroid gland and causes autoimmune hyperthyroidism. In this, thyroid hormones secreted by an overactive thyroid gland speed up the body’s metabolism, causing unexpected loss of weight. People of all ages are affected by Graves’ disease. It is a leading autoimmune endocrine disease affecting females more than males. It is a condition in which the body’s immune system creates autoantibodies and assaults the thyroid and pituitary glands, resulting in excessive thyroid hormone production. The cause of this immune system failure, however, remains unknown.