Gougerot-Sjögren’s syndrome (GSS) is an immune disease primarily affecting the exocrine glands. Due to lymphocytic infiltration of the salivary or lacrimal glands, or sometimes both, the main clinical manifestations are dry saliva and/or dry eyes. Dentists are generally called in to treat complications and oral discomfort caused by instability in the quantity and quality of saliva. The dentist plays an important role in the discovery and early diagnosis of this disease. He can prevent complications by educating patients about oral hygiene and monitoring the progress of the condition.
A little history
The syndrome was first described by the Polish surgeon Mikulicz Radecki, who in 1892 described a patient with bilateral swelling of the parotid and lacrimal glands with a mononuclear infiltrate. Gougerot individualised this syndrome in 1925, grouping together all dry mucous membranes. He attributed it to gland atrophy. In 1933, the Swedish ophthalmologist Henrik Sjögren described the clinical and histological manifestations found in 19 women suffering from dry mouth and dry eyes. Sjögren used the term keratoconjunctivitis sicca to define the eye condition and distinguish it from dry eyes caused by vitamin A deficiency.
What is Gougerot-Sjögren’s disease?
Gougerot-Sjögren’s disease is an autoimmune syndrome characterised by progressive degeneration of the exocrine glands, resulting in dry mucous membranes and conjunctiva. Histologically, the syndrome is characterised by lymphoid infiltration of the exocrine glands, particularly the salivary and lacrimal glands, and the biological production of large quantities of autoantibodies (FAN, anti-SSA, anti-SSB, rheumatoid factor). If the disease appears to be isolated, it is referred to as primary GAS, whereas if there are associated autoimmune diseases (rheumatoid arthritis, systemic lupus erythematosus, etc.), it is referred to as secondary GAS.
The prevalence of primary GSS is estimated at between 0.1% and 0.6% according to the American-European consensus standard. The disease generally affects mainly women (90%) between the ages of 30 and 40.
How widespread is Gougerot-Sjögren’s syndrome in France?
A study published in RMD Open in 2024 has provided valuable data on the prevalence and impact of Gougerot-Sjögren’s syndrome in France. It reveals that this autoimmune disease, which manifests itself mainly as dry eyes and mouth, mainly affects women, with an average age of 60 for primary syndrome and 56 for syndrome associated with other autoimmune diseases. This study highlights not only the increase in cases of this disease but also the associated healthcare costs, highlighting the economic impact on the French healthcare system. This information is essential for understanding the extent of Gougerot-Sjögren’s syndrome and the need for appropriate treatment.
What is the impact of autoimmune diseases on children of African descent?
In an in-depth study published in 2024 in thePediatric Rheumatology Online Journal, researchers examined mixed connective tissue autoimmune diseases and other autoimmune diseases in children of African descent in the French West Indies. Over a period of 23 years, 16 patients were included, with an incidence of 0.23 cases per 100,000 children per year. The mean age at diagnosis was 11.9 years. The study revealed that the main complication was symptomatic pulmonary arterial hypertension, observed in 25% of patients. Most patients received steroids and 88% required steroid-sparing therapy. Three patients developed systemic lupus erythematosus after more than 10 years of follow-up. No deaths or chronic organ failure were reported. This study represents the largest paediatric cohort of Afro-descendant patients treated for these diseases in a high-quality care setting.
How does this disease develop?
This disease generally occurs in subjects with a genetic autoimmune predisposition characterised by a high prevalence of HLA haplotypes B8 and DR3. In this specific environment,damage to the epithelial cells of the exocrine glands, secondary to a viral infection, leads to the development of chronic inflammation, characterised by infiltration of lymphocytes composed of T lymphocytes and B lymphocytes, and the formation of germinal centres. This inflammation will be self-sustaining, causing the gland to malfunction and eventually to be destroyed.
What are the mechanisms behind dry mucous membranes?
The destruction of the glands alone cannot shed light on this dysfunction. At the start of the disease, lymphocyte infiltration is focal and some glands are still intact. Moreover, there is no correlation between lymphocyte infiltration and changes in salivary flow. The remaining glands may, however, malfunction, causing discomfort; this malfunction is thought to be due to abnormalities in the autonomic nervous system, which controls, among other things, lacrimal and salivary secretion. Since the autonomic nervous system does not do its job properly, this deficiency could be linked to autoantibodies that turn against M3 muscarinic receptors (which control water secretion from the lacrimal and salivary glands via membrane expression of aquaporin 5, which also appears to be defective in the case of GAS).
Ultimately, dryness would be due to glandular destruction, but also to a deficit in the autonomic nervous system and a defect in the membrane expression of aquaporin 5. These pathophysiological findings open up interesting prospects for the treatment of GSS.
What are the symptoms of Gougerot-Sjögren’s disease?
Symptoms are dominated by ocular and oral involvement, which are common in 90% of patients with GMS. Patients complain of difficulty swallowing, a lack of stability in removable dentures, the appearance of cavities, chronic burning of the oral mucosa, intolerance to spicy or acidic foods, an inability to eat dry foods or to speak continuously for several minutes.
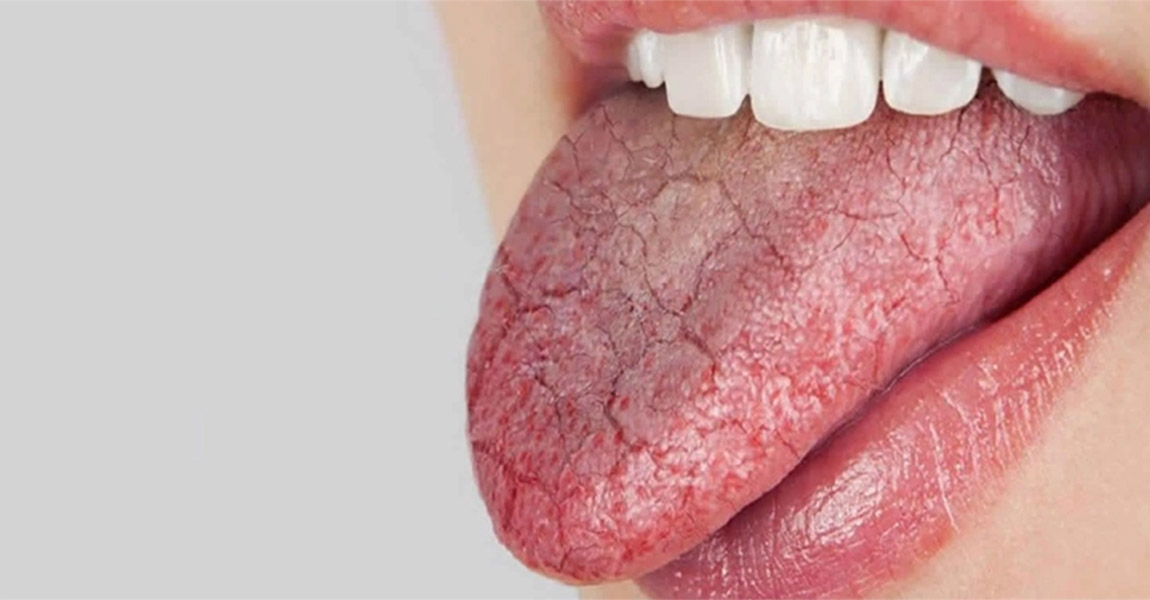
The onset of symptoms is insidious and progresses slowly. The oral mucosa becomes dull, sticky and fragile. The tongue is red, depilated and cracked , and the saliva lake usually present on the floor of the mouth is often non-existent.
Candidiasis is therefore very common in GSS, affecting up to 70% of patients and presenting in a variety of forms:acute pseudomembranous candidiasis (thrush), erythematous candidiasis, angular cheilitis (perlachia), subprosthetic stomatitis, etc.
What naturopathic advice do you have for reducing the symptoms of autoimmune Gougerot-Sjögren’s disease?
If you suffer from autoimmune Gougerot-Sjögren’s disease, you know how difficult the symptoms can be to manage. However, there are a number of steps you can take to improve your quality of life. In this part of the article, we’ll give you some naturopathic advice on how to reduce the symptoms of autoimmune Gougerot-Sjögren’s disease. These measures can be used alongside the medical treatment prescribed by your doctor to improve your general well-being.
Avoid mucosal drying environments:
Learn to recognise and avoid places with low humidity (shops and offices with air conditioning),exposure to wind, dusty places, irritating substances and cigarette smoke.
Taking care of your oral and dental hygiene:
Oral hygiene must be rigorous and regular!
- Brush your teeth after every meal with a soft surgical toothbrush and fluoride toothpaste.
- Choose a non-aggressive mouthwash (bicarbonated water).
- Use dental jets and periodontal floss to clean the interdental spaces.
- Systematically clean and brush removable dentures, which should be placed in an antiseptic solution every night.
The role of water :
Replacing the missing secretion can be easily achieved by taking frequent sips of water. The water does not have to be swallowed, but can be used as a rinse. However, water does not adequately moisten or lubricate the oral mucosa and teeth.
Stimulate your salivary secretion:
When residual salivary secretion is high enough, chewing sugar-free chewing gum is a good stimulus. If it is insufficient, the chewing gum will stick to the teeth. Sucking dried fruit such as peaches and nectarines can also stimulate saliva secretion.
Are there any natural treatments to stimulate the exocrine glands?
Treatment is adapted to the severity of the symptoms. The clinical picture is highly variable, ranging from asymptomatic to very severe. Most patients with GSS require only local treatment for dry syndrome. As a general rule, drugs that may aggravate dry syndrome should be avoided (retinoids, beta-blockers, antihistamines, etc.). The main aim of treatment is to improve patient comfort.
Artificial saliva :
There are several artificial saliva products containing methylcellulose; some contain animal mucin to reduce viscosity. They are available in various galenic forms (liquid, lozenge or chewing gum). There are also other saliva substitutes such as polyethylene oxide or polysaccharide extracts from flaxseed.
The former appears to be more effective than methylcellulose in reducing the symptoms of xerostomia, while the latter gives satisfactory results in around 75% of patients. Products based on polyacrylic acid and xanthan gum have been developed and evaluated in patients with GAS. This latest study showed that there are subgroups of patients in whom a particular form of substitute is more clinically effective. Highly mucoadhesive polymers such as polyacrylic acid are recommended for patients with extremely low salivary flow.
On the other hand, patients who still have moderate salivary flow show more improvement with substitutes that have moderate mucosal adhesion and good elastic properties (xanthan gum). In fact, these polymers improve the physico-chemical properties of residual saliva, resulting in increased humidification and lubrication. Residual saliva secretion is stimulated by non-specific mechanical or gustatory stimuli. Citric acid, for example, stimulates taste, while chewing gum stimulates both.
Jaborandi mother tincture:
The pilocarpine naturally contained in Jaborandi officinal is a cholinergic muscarinic receptor agonist. Its mechanism of action is to increase salivary secretion and, to a lesser extent, lacrimal secretion.
Replacement eye drops :
The treatment of dry eye syndrome essentially involves the use of artificial tear substitutes.
Medical literature and clinical trials:
- Kassan SS, Moutsopoulos HM. Clinical manifestations and early diagnosis of Gougerot-Sjögren syndrome. Arch Intern Med 2004
- Mariette X. Pathophysiology of Gougerot-Sjögren syndrome. Ann Med Intern 2003
- Moutsopoulos HM. Sjogren’s syndrome: autoimmune epithelitis. Clin Immunol Immunopathol 1994
- Fox RI. Sjogren’s syndrome. Lancet 2005
- Steinfeld S, Cogan E, King LS, Agre P, Kiss R, Delporte C. Abnormal distribution of aquaporin-5 water channel protein in salivary glands from Sjogren’s syndrome patients. Lab Invest 2001
- Gentric-Tilly A. Gougerot-Sjögren’s syndrome in the elderly. Ann Med Interne 2002
- Korsten MA, Rosman AS, Fishbein S, Shlein RD, Goldberg HE, Biener A. Chronic xerostomia increases esophageal acid exposure and is associated with esophageal injury. Am J Med 1991
- Vissink A, De Jong HP, Busscher HJ, Arends J, Gravenmade EJ. Wetting properties of human saliva and saliva substitutes. J Dent Res 1986
- Johansson G, Andersson G, Attstrom R, Glantz PO, Larsson K. The effect of Salinum on the symptoms of dry mouth: a pilot study. Gerodontology 1994
- Van der Reijden WA, van der Kwaak H, Vissink A, Veerman EC, Amerongen AV. Treatment of xerostomia with polymer-based saliva substitutes in patients with Gougerot-Sjögren syndrome. Arthritis Rheum 1996
- RMD Open. 2024; Estimated prevalence, incidence and healthcare costs of Sjögren’s syndrome in France: a national claims-based study
- Pediatr Rheumatol Online J. 2024; 22: 13. Longitudinal follow-up of mixed connective tissue disease and overlapping autoimmune diseases of childhood onset in the Afro-descendant population of the French West Indies