Osteoarthritis is the most common rheumatic disease in Western countries. It would affect 9 to 10 million French people (17% of the population).
What is osteoarthritis?
Definitio n: Mechanical and non-inflammatory joint disease, characterized by degenerative joint damage, associated with a proliferation of underlying bone tissue. Osteoarthritis is a disease of the joint and not just of cartilage. About half of those affected by osteoarthritis are symptomatic. It is very common after age 65 and is the second leading cause of disability after cardiovascular disease.
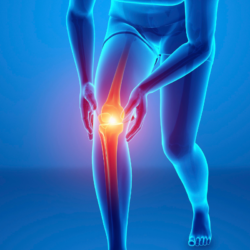
Goa rthritis or osteoarthritis of the knee, along with digital osteoarthritis and osteoarthritis of the hip, is one of the 3 major locations of osteoarthritis. It may involve the joint between the patella and the femur (femoro-patellar osteoarthritis, 35% of cases) or the joint between the femur and the tibia (femoro-tibial osteoarthritis, 45 to 50% of cases), these two forms are sometimes associated (15 to 20% of cases)
The causes of osteoarthritis
Even if you get older, the more likely you are to suffer from osteoarthritis, aging is not the cause. Osteoarthritis can develop in a young person, even in adolescents with cartilage abnormalities.
In addition to age, which is an aggravating factor in osteoarthritis, various factors contribute to the occurrence or worsening of osteoarthritis:
- Bone or joint diseases. These diseases affect the quality and quantity of cartilage (Paget’s disease, diseases causing deposits in the joints.
- Anatomical malformations: congenital hip luxitization, X-shaped or knee barrel deformity, scolioses…
- Genetic terrain. There are family predispositions to develop osteoarthritis
- Overweight, trauma (fractures, sprains, professional micro-traumas, some intensive sports…)
Ch anges in the joint during osteoarthritis or pathophysiology
Normally, cartilage forms a flexible gel that ensures slippage and mobility of the ends of the bones between them in the joint. It renews itself throughout life. But when the mechanism of removal of worn cartilage debris and repair by specialized cells (chondrocytes) is unbalanced, the cartilage degrades, loses its elasticity, cracks and secretes a substance causing an inflammatory reaction of the synovial membrane that surrounds it and pain.
- When it becomes arthrosic, the cartilage turns brown and disappears in certain areas that hint at the subchondral bone. Histologically, it becomes fibrillary or even cracked with decreased number of cells and loss of arrangement. Chondrocytes (cartilage cells) have a wide variety of phenotypes, sometimes leading to cell death.
- At the same time, after an initial phase of edema, the amount of water decreases and the “water pocket” effect disappears explaining the alteration of the biomechanical role of cartilage.
- A disruption of the behaviour of chondrocytes gradually takes hold, resulting in an imbalance between the synthesis and degradation of matrix components and cartilage resistance abilities gradually diminishing.
- There is a thinning of the layers of cartilage that eventually disappears.
- Condensation of the subchondral bone is observed and this osteocondensation helps to decrease the shock absorption capabilities to which the joint is subjected. The production of bone growth at the margins of the joint (osteophytes or “parrot beaks”) could correspond to an attempt by the aberrant repair organism.
- Finally, the synovial membrane is prone to episodes of inflammation that can clinically result in the presence of an intra-articular effusion
|
Initial stage |
Intermediate stage |
Final stage |
| Edématiated cartilage |
|
|
Wh at are the clinical signs of osteoarthritis?
| Pain | That’s the first sign. It is triggered by the loading or operation of the joint. At first, she appears in motion only, yielding to rest. The pain disappears at night and does not wake the patient except to changes in position. At an advanced stage, the pain becomes chronic. |
| Stiffness | or limitation of joint play: it varies depending on the joint. Appearance of morning stiffness requiring a few minutes of diversion (usually less than a quarter of an hour) |
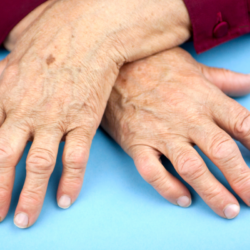
| Deformities and swelling | The swelling is related either to the accumulation of synovial fluid that inflates the joint cavity, or to a thickening of the tissues of the joint and/or the appearance of osteophytes. |
| Crunches | They accompany the pain. At first, they are not painful but can become painful as the cartilage degrades. |
Ca n osteoarthritis be cured?
A study in Canada appears to show that cartilage damage can be seen regressing. It can even heal completely (normalization of microscopic and biological examinations)
This type of healing has been almost constantly observed with a certain type of treatment: “effortless movement” (52% healing). However, this healing takes time (at least 12 weeks).
How to avoid osteoarthritis?
The architecture of cartilage can be compared to that of a mattress whose springs provide it with strength, elasticity and compressibility. In the physiological state, cartilage is an extremely quiescent tissue (whose cells divide very little).Its renewal is almost nil for collagen fibers and takes several hundred days for proteoglycans. That’s why you have to spare your joints by following the tips below.
Tips on osteoarthritis
A dapting a good diet
- Fighting overweight.
- Promote a diet rich in antioxidants to limit the effects of aging; A diet rich in fruits and vegetables (antioxidants), pulses (lentils, peas, white beans), fish, olive oil (not to cook with butter) and whole grains. Foods rich in omega 3 have analgesic and anti-inflammatory properties (Argan vegetable oil, hazelnut oil, oily fish, etc.). An Omega-3 supplementation is interesting: CardioConfort® Omega-3, Arkogélules flaxseed oil®
- Reduce protein and dairy products (rich in protein and omega 6) that acidify the blood and increase joint pain.
Ad apting a healthy lifestyle
- “Go yes, overmen-no.” Physical activity helps maintain the tone of the muscles and tendons and thus stabilizes the diseased joint. It also helps to promote the diffusion of nutrients inside the cartilage. for example, cycling, swimming, walking (at least 30 minutes every 2 days). Avoid sports activities that put a lot of pressure on the joints (for example, jogging on bitumen, tennis). Prefer regular terrain to uneven terrain. In the event of a flare-up, the joint should be put to rest, but as soon as it is finished, it is necessary to become active again, even if some pain persists.
- Do not smo ke because tobacco inhibits cell proliferation within cartilage. It caused oxidative stress that would eventually wear out the joints. In addition, carbon monoxide from the burning of cigarettes circulates in the arteries and also contributes to the loss of cartilage.Reumatology (Oxford), October 2009; 48(10) 1227-3
Adapt good posture and dress
Change your body position regularly. Avoid sitting and standing for long or in any other position that overloads the joints, such as long drives. Avoid kneeling
- At rest, put the joints in a comfortable p osition: the knees and hips extend; it may be more enjoyable to lie down with bent legs (resting chairs) Relaxing painful joints helps reduce pain. Sitting, stretch your legs
- Avoid overloading the joints, which would only increase the pain. Pain is a sign of overload on the joint.
- Don’t carry heavy loads
- Wear com fortable shoes th at hold the foot without tightening it, such as shoes with elastic laces and thick cushioning soles. Prefer wide, low heels with the terminal edge of the bevelled heel (to make it easier to run the step smoothly).
- Avoid shoc ks when walking: use shock absorbers at the heel (silicone heels), have a good insole (sole with plantar arch).
- Prefer wa rm wool clo thing preferably. There are also heated items (socks, belts, collars, shoulder pads, elbow pads, knee pads, wrists: Gibaud Thermotherapy range, Heating Pack (Geo® Hot/Cold Pack)
How to treat osteoarthritis
The management of osteoarthritis is primarily aimed at relieving pain, improving mobility and, if possible, slowing down cartilage degradation.It is recommended to wait 3 or 4 months before judging the effectiveness of a treatment. The effectiveness may persist for several weeks after discontinuation of treatment.The interest of the association of several antiarthrostics is not demonstrated, and the optimal duration of treatment is not known
Treatment of osteoarthritis
Ba ckground treatment with slow-acting antiarthrosics
Dia cerheine
Diacerhine is an interleukin-1 inhibitor (IL-1) whose effects are similar to those of TNF. In fact, IL-1, mainly produced by monocytes, macrophages and cells of the synovial, bone and cartilage, is a powerful pro-inflammatory (it stimulates, among other things, the synthesis of inflammation proteins, collagens and proteoglycanases destroying the cartilage matrix and inhibiting the multiplication of chondrocytes). It stimulates the production of growth factors such as TGF-beta
According to studies, if the response to these therapies is not apparent at 6 months, a positive effect may appear after 2 or 3 years of treatment. It is therefore essential to take these medications in the long run.
Taking in the middle of meals improves its bioavaila bility
Common side effects: diarrhea, soft stools and abdominal pain. Risk of dehydration in the elderly and/or under diuretic
Soy an d avocado extracts
Piasclédine stimulates the production of growth factors such as TGF-beta and by this phenomenon prevents the destruction of cartilage.
Rare side effects: l ipid-smelling regurgitations. To avoid this, it is best to take the medication in the middle of a meal.
Gl ucosamine
Glucosamine is a normal component of the polysaccharid chains of the cartilage matrix and synovial liquid glycosaminoglycans. Its production decreases with age.
It is hydrolyzed from crustacean shell chitin and indicated to relieve symptoms associated with mild to moderate knee osteoarthritis at dosages in the range of 1200 to 1500mg/day
2 tablets a day to take during or outside meals.
Contra indic ated in people allergic to crustaceans. Use with caution in case of anticoagulant treatment with warfarin (risk of potentiating the effect of AVK)
Caution in diabetics (deterioration of possible glycemic contr ol)
Generally mild and transient side effects: nausea, abdominal pain, digestive disorders, headache, rash, fatigue and pruritus
Chond roine sulfate
The mechanism of action of chondroin is mainly anabolic (inhibition of elastase, mediator of cartilage degradation). It stimulates the synthesis of proteoglycans by cultured chondrocytes.
Recommended dosage: 2 capsules per day.
Rare side effects, mai nly skin effects
Pain tr eatment
Oral
Non-opioid painkillers (Palier I): aspirin, Paracetamol (Dolipraneoro), nonsteroidal anti-inflammatory drugs (Ibuprofen
Advil, Advilcaps, ADVILEFF, Gelufène, Spedifen Nurofenflash,Nurofen, Nureflex, Spedifen), naproxen, ketoprofen, diclofenac, celecoxib -Celecoxib – Celecoxib, etoricoxib arcoxia).
- Weak opioid painkillers (palier II): codeine, dihydrocodeine, tramadol (Ixprim , Zaldiar)
- Strong opioid painkillers (palier III): morphine and morphinic derivatives . Reserved in case of rebellious pain to other treatments.
- Anticonvulsants (lyrica,Neurontin) work by inhibiting the transmission of neuronal pain.
Local lane
NSA (diclofenac 1%) in gel form or in the form of a bioadphesial device: Flector fabricgel, Voltarenplast . Their effectiveness is increased if used in the form of occlusive dressing. Renew the app every 12 hours. They are compatible with wearing an orthotic.
-
Application of a revulsive (heating cream, heating patch…):For more information visit our advice section:Hot Patches
Actipoche, Aroma Patchs, DOLPIC, Elastoplast patches, Nexcare Heating Patchs, Synthetic Heating Patchs, Thermacare, URGO Heating Patch, VoltaCare Heating Patchs, Puressential Joints Patch, American St. Bernard, Cryo Liner/Universal Thermo, Cervico Cherry Core
-
Orthotics: immobilization of painful joints has analgesic action
In tra-articular injections
Intra-articular injections of hyaluronic acid (Altim, Hyalgan, Synvisc, Euflexxa, Go-on…).These viscoelastic solutions are composed of polysaccharide (glucuronic acid – N-acetylglucosamine) used in the composition of cartilage and synovia.The injections are performed at a rate of 1 per week for 3 to 5 weeks. It is a visco-replacement because the injected substance lubricates cartilage, absorbs mechanical shocks, promotes greater mobility and thus reduces pain.
Arthritis and nutritherapy
Ma ny dietary supplements can relieve the pain associated with osteoarthritis and help prevent joint breakdown. They are to be taken on cures of at least 3 to 6 months to have an improvement.
Substances useful to joints:
Glucosamine (Arthrobiane on Care and Nature)
Glucosamine is an amino sugar that serves as a substrate for the synthesis of glycosaminoglycans used to synthesize cartilage. It is made by the body from glucose and an amino acid: glutamine. In the laboratory, it is obtained from shells of crustaceans.
Mechanism of action:
- This substance, normally manufactured by the body, allows cartilage to absorb shocks. They help retain water molecules, thus ensuring the hydration of the cartilage. Linked to proteins, they form proteoglycannes that can be likened to sponges trapped in a tight mesh network (network of collagen fibers). The elasticity of cartilage is favoured by the hydrophilia of proteoglycannes which allows a movement of water molecules back and forth during the mechanical loads of the joint.
- A single intake of 1500mg/d (corresponding to 1250 mg of free glucosamine) causes inhibitory effects on the activation of NF-B involved in the cartilage degradation chain, but also in the synthesis of certain mediators of inflammation type prostaglandin E2 (IL6, IL8, TNF and NO).
Precaution of use:
- Not recommended if you are taking blood thinners as it increases the risk of bleeding.
- According to some studies, glucosamine may cause insulin resistance. Its use is therefore strongly discouraged in people with diabetes or obese.
Side effects: nausea, diarrhea, abdominal pain, rashes
C hondroine sulph ate
Chondroin is obtained from fish cartilage (e.g. sharks), it is present in many medicines. This component of the cartilage matrix serves as a chondromodulator agent in protecting cartilage from enzymatic reactions and damage due to free radicals.
Clinical studies have suggested its effectiveness in preventing the progression of osteoarthritis.
Simultaneous glucosamine intake may amplify its effect.
Against indicat ions: Allergy to crust acean s
O mega 3
Omega 3 polyunsatu rated acids reduce inflammatory processes.
However, medical advice is recommended for patients on anticoagulants.To learn more about omega 3, check out our advice sheet: Omega 3
H yaluronic acid
Naturally present in the skin, hyaluronic acid provides a large part of the hydration, elasticity and tone of the joints, derme and epidermis, it also has a volumizing effect.
Co llagen
Collagen is a fibrillary protein naturally made by the body that guarantees the flexibility and elasticity of joints and skin. Its production naturally decreases by 1% per year from the age of 30
Vitami ns and mine rals
Vitamins C,D,E: In their absence, osteoarthritis develops more rapidly.
Prefer the natural vitamin C that is acer il a
Magnesium and ma nganese also play a protective role against the development of osteoarthritis
Silicon, copper and zinc are antioxidants and help fight joint aging
Sulphur (methy l sulfo nymethane) would help maintain connective tissues, including cartilage and tendons, in good condition. Sulphur is contraa indicated in case of kidney problems.
Pl ants
T urmeri c
Turmeric in standardized plant ext ract (Curcuma A rkogélule®) is a natural anti-inflammatory and a powerful anti-oxidant to better fight against joint aging.
Nett le
Nettle is a remineralizing plant, very useful in osteoarthritis.
Other plants: w hite willow, harpagophytum, blackcout……
Find out more about plants that relieve osteoarthritis in our Osteoarthritis Herbal Therapy section
Silica, Silic on
Silica allows cartilage to regenerate.
Bamboo and nettle are naturally rich in silica.
Silicea 1DH powder: Dilute a measuring spoon in a 3/day water base.
Arthritis and homeopathy
Warning. The following treatments are given only as an indication. Only a homeopath doctor can prescribe a treatment that is truly appropriate for you
Bac kground treatment
- Rhus tox compound: 3 granules 5 to 6/day
- Alternate: Cartilage D8 and Medullos D8 at the rate of one bulb every other day in sublingual
- Apply a Gel of Arnica 2 to 3 times a day: Arnican gel, Arnigel or Bio Arnica Gel
Tr eatment of arthrosic pain
Depending on the symptoms at the beginning:
- Arnica montana Caused by a movement or a fall, feeling of having received a shock. Feeling of generalized aches and pains. Former force workers
- Rhus toxicoden dron Feeling stiff, improved by slow movement. Aggravation at rest. The tendons the ligaments of the joint are susceptible to palpation. Sharp aggravation by the wet cold, by prolonged rest and lying on the painful side. Improved by hot applications.
- Ruta graveole ns pain disappearing the day. Aggravated by rest, improved by movement. Treatment of sprains and ligament weaknesses
- Feeling of muscle stiffness, cramps, spasms – A ngustura vera 7CH
- Pain with difficulty turning, tear-pulling sensation – Nux vomica 7CH
- Bryoni a Improvement at absolute rest with fresh articulation, and aggravation to movement. Swollen, hot and red articulation with acute nagging pain. The skin is tense shiny, signifying the likely presence of a synovial effusion. Complete Apis (faster but shorter)
- Api s: swollen, shiny, sensitive, sore, painful, pungent, stinging, burning joint, enhanced by cold applications, aggravated by heat.
- Kalium ioda tum: periost pain with a tendency to hydarthritis; improvement by movement, night worsening and touch
- Palustre Led um: swollen, pale or purple and strained joint. Pain improved by cold applications. Aggravated at night and in the heat of the bed. Pains evolving from bottom to top.
- Petro leum: bruising sensation at the joint, with joint cracking. Meniscal lesions.
- Pulsati lla: swollen joint, purple pink with pulling pain
- Dulcama ra: aggravated rheumatic pain at rest, improved movement, mainly muscular. Hydrogenoid, hypothyroid, sycotic subjects often with alternating rashes and rheumatic pain.
- Pain aggravated by cold and water.Urticary, Drop – U rtica urens 7CH
- Radium bromatu m: joint pain with the feeling that the bones will come out.
- Sticta pulmonar ia: synovitis, bursitis, hygroma joints alternating with colds
Treatments to be taken in 7 CH. Suck 3 granules 3 to 5 times a da y
At the state period
The joints are permanently painful and already deformed, lipomatous, with significant radiological alterations. It is then necessary to seek constitutional treatment among:
Sulfur: sulphur especially in the evening and at night, with swaying pains, pulling
Kalium carbonicum: pungent pain felt both at rest and while moving, aggravated lying on the painful side, cold and at 2 or 3 in the morning
but still, according to the similarities, look for a treatment among: Calcarea carbonica, Calcarea phosphorica, Calcarea fluoride, Causticum,Luesinum, Medorrhinum, Tuberculinum, Thuya…
Cervicarthr itis
Pain in the cervical vertebrae – Rhus toxicodendron, Lachnantes 7CH, Cervical Disc D8, Arnord N erve D8
Gothring
Knee pains as you climb or down stairs: Badiaga
Left knee pain: Heliantus
Cracks in the knees: Crocus
Feeling of knee contracture, pungent pain, especially in angina suites: Guaiacum
Spina l arthritis
Green disc D8, Meduloss D8
Lomba rthritis
Lumbar disc D8, Sciatic Nerve D8
Anxiety and herbal medicine
Osteoarthritis is a chronic disease that requires long-term treatment. Some of these treatments, such as anti-inflammatory drugs, are sometimes poorly supported. Plants offer an interesting natural alternative in the treatment of osteoarthritis.Mech anism of action
Plants help relieve osteoarthritis by acting on three axes:
- Remineralizing Action: Remineralizing plants help restore arthrostic joints
- Anti-inflammatory ac tion: anti-inflammatory plants reduce pain, as well as inflammation that self-maintains cartilage destruction
- Desormintive action: Deering plants cleanse the body and eliminate toxins often causing inflammatory mechanisms
Re mineralizing plants
Horset ail
The sterile aerial parts of the prêle have a remineralizing and trophic effect. The prêle has a high silica content (5 to 10% of the dry plant). Silica plays an important role in maintaining and renewing connective tissue (collagen synthesis). It would promote the metabolic absorption of calcium.
- 2 capsules at 400mg in the morning, or
- Take 2 to 3g of plant/d (aerial parts, powder, liquid extract, dry extract). Prolonged decoction of dry aerial parts
Do 20-day-a-month cures. The effect is maximum in 3 months cure.
Li thotame
Lithotame: seaweed that crystallizes marine minerals on its thalle, mainly calcium (contains 25-30% calcium in the form of carbonate), but also magnesium and iron. Take 3g/d.It is known for its remineralizing and anti-rhyming properties, fighting against the excess acidity produced by the body which constitutes a favorable terrain for joint pain. The combination with the prêle is possible.Attention because of its richness in iodine, this plant is not recommended in case of hyperthyroidism.
Ba mboo
The bamboo stem has a high natural silica content (between 60 and 70%). Silicon is one of the most important compounds of connective tissues. He is involved in calcium fixation, collagen and proteoglycannes synthesis, as well as bone formation. It also has an anti-inflammatory action. This plant contributes to the comfort of the joints and helps prevent cartilage degeneration.The effect is maximum per 3-month cure
Anti-inflammatory plant s
Ha rpagophytum
The harpagophytum root is still called the “devil’s claw.” It is rich in harpagoside procumbide, powerful anti-inflammatory and analgesic and hargid. It is traditionally used in the symptomatic treatment of minor painful joint manifestations, whether of rheumatic, arthrostic or traumatic origin.It is co ntraindicated in cases of pregnancy, breastfeeding and gastoduodenal ulcer, it can cause gastrointestinal disorders.Do not associate with anti-inflammatory drugs.For relief from musculoskeletal pain and arthralgia treatments should be extended for at least 3 weeks on average. A take over several months is possible.
Queen of the M eadows
The queen of meadows is interesting especially for rheumatism aggravated by humidity. Attention the queen of the meadows contains a salicyle derivative (salicyne), and is contraindated in case of duodenum ulcer, in pregnant women and in case of breastfeeding.
Infusion of 50 g of flowering luminaries (flowers less than one year old) per litre of water, leave to infuse for 10 minutes, or take 1 teaspoon of fluid extract for a background anti-inflammatory acti on
Willow
Willow bark is an anti-inflammatory plant.Decoction of 20 to 30 g of willow bark per litre of water. Drink 2 to 3 cups a day before meals.Beware the willow contains a salicyle derivative (salicyne), and is contraindated in case of duodenum ulcer, pregnant woman and in case of breastfeeding.
Bl ackcur rant
Blackcover leaves are rich in flavonoids and vitamins C and P.This plant has an anti-inflammatory action coupled with a diuretic action that promotes the elimination of waste from the body (uric acid, lactic acid, toxins…). It can be used against gout, but also in cases of rheumatic diseases.
Tips for use: Make an infusion of 50 g of cassis leaves per litre of water. Leave to infuse for 10 minutes and take 3 cups a day between meals, or take 2 cassis SIPF caps per day diluted in a glass of water.
Sc rofular
This plant has anti-inflammatory properties. It contains the same active ingredients as harpagophytum (harpagoside and hargide) It is used to alleviate rheumatic pain and osteoarthritis.As a precautionary measure, scroludoment is not recommended during pregnancy and breastfeeding, in children and in cases of peptic ulcers.
Use: decoc tion of 15 to 20 g of root per litre of water for 10 minutes; drink 2 cups a day.
Counter-indicati on: Association with warfarin and anti-arrhythmics. Contra indicated in case of insufficiency.
Bo swellia Serrata
Boswellia, also called oliban or incense, is a plant native to Africa or Asia, known for its anti-inflammatory properties. The main active component is Boswelic acid.This plant has been the subject of several studies that have shown efficacy in inflammatory diseases such as arthritis, ulcerative colitis and asthma.We use the resin of this plant.The dosage found is 150 to 200 mg 3 times a day of extract containing at least 60% of Boswéliques acids.4 to 8 weeks may be necessary to feel the therapeutic effects.Counter-indication: Pregnancy.A January 2003 study in India of 30 people with osteoarthritis of the knee tested positive after 8 weeks of Boswellia treatment. Boswellia extract was significantly more effective than placebo in reducing pain, improving knee flexibility and increasing walking distance.
Pl ants that are both remineralizing and anti-inflamma to ry
Nettle
Aerial parts of nettle are rich in calcium and silicates (organic silicon). They have long been used as a diuretic and against joint or rheumatic pain externally, but also internally.
This plant would cause partial inhibition of 5-lipoxygenase, cyclooxygenase, inhibition of the synthesis of leucotriene B4 and prostaglandins, inhibition of T-cell cytokines; mediators of pain and the inflammatory process. This plant has an action that can prevent this inflammatory cascade in autoimmune diseases…
Use:
Infusion 30 to 60 g of leaves (Green mark® Hot nettle) per litre of boiling water.Leave to infuse for 10 minutes. Take a cup 2 to 3/day before meals, or capsu les (Arkogélu les®)
Pharmacy Tip: When to see a doctor
- In case of acute, recent hyperalgic pain
- If the diagnosis has not been made